Hyphema eye paracentesis (Video)
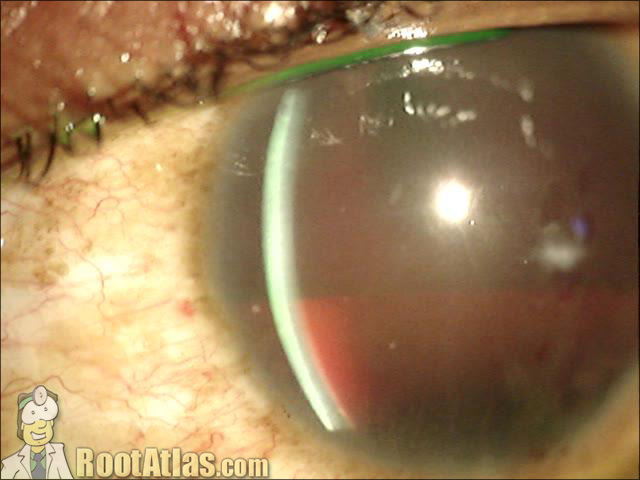
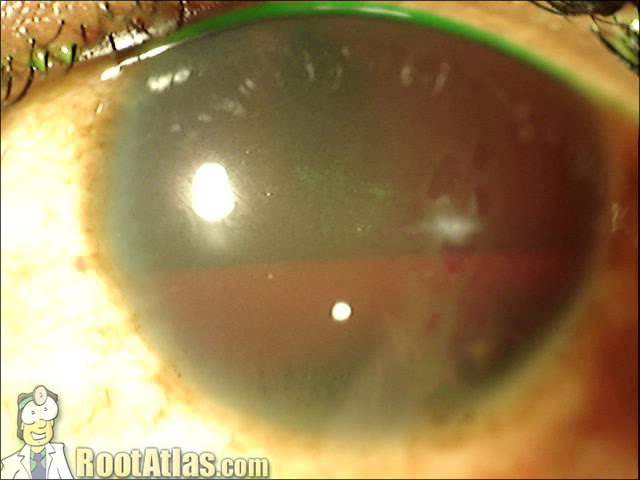
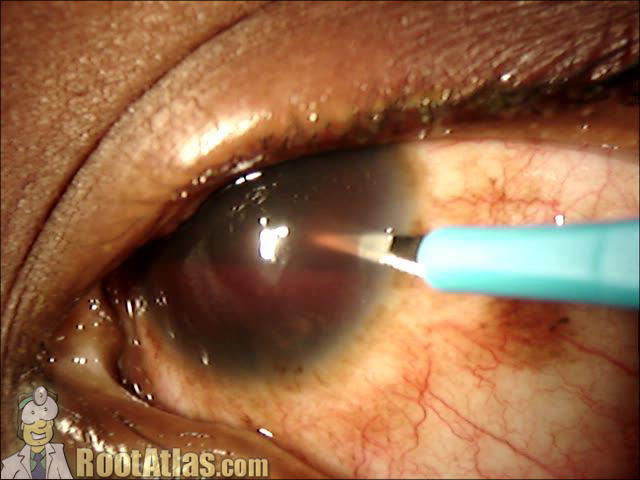
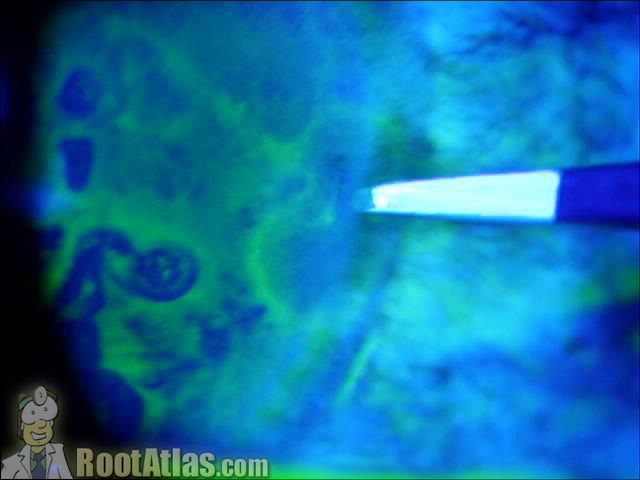
This video shows an eye with a large hyphema (blood) inside the anterior chamber. The blood has settled into the bottom 35% of the eye, while the upper portion of the AC is dense with free-floating RBCs. In the last half of the movie, I create a paracentesis using a super-blade scalpel.
Hyphemas typically occur secondary to blunt trauma, and occasionally after surgery. They will absorb eventually, but the concerns in the immediate post-bleed period is:
1. Pressure: The blood clogs up the trabecular meshwork and the pressure can become very high in the eye, and compromise the optic nerve. Treat aggressively with aqueous supressants (beta-blockers) and perform a paracentesis if needed.
2. Blood staining: If the pressure is too high for two long, the inner cornea can be stained with blood. This staining may go away after years, but it can take a long time and affect vision. Decrease the pressure, and perform an AC washout if staining seems imminant.
A couple more points
- Avoid CAIs in anyone who might be sickle-cell as this acidifies the AC and promotes sickling
- If you’re going to use an oral CAI, use methazolamide instead as it affects the pH less
- The re-bleed danger time is 3-5 days as this is when the clot retracts. Follow daily during this time period to watch the pressure
- A paracentesis can lower the pressure acutely, but may also cause a rebleed as the pressure that was tamponading the bleed is lowered suddenly
- Don’t gonio these eyes until everything has resolved to avoid rebleeding. Many of these eyes will have angle recession from the blunt trauma that may cause glaucoma down the road
Download this video
To download this video, right click on a link below and choose “Save Target As…”
hyphemaparacentesis.wmv (13.7 meg, Windows video file)
Screencaptures
Very helpful clip.
please i want to know more about this small operation for the eyes .thanks.
What are teh possible complications (beside of infection) of performing a paracentesis in this case? thanks.
Fantastic, really very helpful & thanks for creation
the day after cateract surgery a young doctor burped my eye because the pressure was too high. I would like to know if a puncture was made and if the proceedure was necessary. I do not have glacoma.
I’m just an OD student, but I believe the doctor just put pressure on you eye to “burp” it. Excess fluid came out of the existing incision from the cataract surgery. Those incisions are small which are self sealing (no stitches typically) but can be temporarily forced open with enough pressure that soon after surgery.
Realy helpful👌🏻