Chapter 7: Pediatric Ophthalmology
Pediatric ophthalmology is a fascinating field, but can be frustrating for many residents because children are hard to examine. Despite this challenge, pediatrics is rewarding and is one of my favorite sub-specialties.
The Pediatric Exam:
Examining kids is a difficult prospect, as children are moving targets and universally hate strangers messing with their eyes. You have limited time before your child further decompensates, so it’s important to hone in on any eye problems quickly.
 Vision testing also depends upon the age of your patient. Young babies may only blink-to-light, but as the child gets older they start to track faces, and eventually identify pictures. It’s hard to measure quantitative vision in the young, so focus on asymmetry between the eyes. For example, cover each eye and watching how the child reacts and tracts. If a baby is fussier with a particular eye covered, then you may be covering his only good eye! Also, toddlers will cheat when covering the eyes, so watch them closely!
Vision testing also depends upon the age of your patient. Young babies may only blink-to-light, but as the child gets older they start to track faces, and eventually identify pictures. It’s hard to measure quantitative vision in the young, so focus on asymmetry between the eyes. For example, cover each eye and watching how the child reacts and tracts. If a baby is fussier with a particular eye covered, then you may be covering his only good eye! Also, toddlers will cheat when covering the eyes, so watch them closely!
Refractive Error
Determining a child’s refractive error is even more challenging … how can you tell if a child is myopic or hyperopic when they can’t read the eye chart? Here’s how we do it:
Bruchner Test:
 One quick method to estimate refractive error is by examining the red-reflex (the red-eye you get in photographs). Hold a direct scope from a distance and shine it so that the circle of light lights up both pupils at the same time.
One quick method to estimate refractive error is by examining the red-reflex (the red-eye you get in photographs). Hold a direct scope from a distance and shine it so that the circle of light lights up both pupils at the same time.
Examine the red-reflex from each eye. Assuming that the child is looking right at you, the placement of the red-reflex gives some clues. Inferior crescents, such as in this drawing, indicate myopia (near-sightedness) while superior crescents indicate hyperopia.
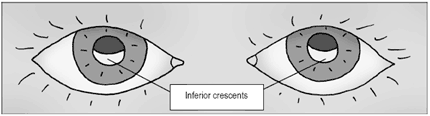
Most children have some degree of hyperopia, as their eyes are small and still growing. This makes the Bruchner test more useful for picking up myopic (near-sighted) errors, but overall the test isn’t very accurate in undilated children as they have the ability to accommodate. Also, if the eyes are not well aligned, such as strabismus, the results are inaccurate.
Retinoscopy
 Retinoscopy is a much more accurate way to check prescription, and is how we refract all pre-verbal children for glasses. By flashing a beam of light back-and-forth into the eye we can examine how the light bounces off the retina. By holding different power lenses in front of the eye we can figure out what power lens focuses the light properly and neutralizes the red-reflex. This is a difficult skill to learn, but surprisingly useful, even outside of the pediatric realm.
Retinoscopy is a much more accurate way to check prescription, and is how we refract all pre-verbal children for glasses. By flashing a beam of light back-and-forth into the eye we can examine how the light bounces off the retina. By holding different power lenses in front of the eye we can figure out what power lens focuses the light properly and neutralizes the red-reflex. This is a difficult skill to learn, but surprisingly useful, even outside of the pediatric realm.
Amblyopia (a.k.a. “lazy eye”):
Amblyopia is decreased vision in an eye because of disuse of that eye during childhood development. The prevalence in the USA is 2-5%, the major risk factors being prematurity, developmental delay, and a family history.
The visual pathway is a plastic system that continues to develop during childhood until around 6-9 years of age. During this time, the wiring between the retina and visual cortex is still developing. Any visual problem during this critical period, such as a refractive error or strabismus (misaligned eyes) can mess up this developmental wiring, resulting in permanent visual loss that can’t be fixed by any corrective means when they are older.
Competitive Wiring!
If you don’t use an eye, the nerve fibers from that eye don’t develop … in fact, the eyes are in competition with each other. The afferent nerve connections of the strong eye become numerous while the weak (unused eye) nerves atrophy and decrease in number. In animal studies, occlusion of one eye leads to loss and atrophy of cells in the LGN (lateral geniculate nucleus) associated with that eye.
Fortunately, the situation can be reversed. Penalizing the strong eye, with the use of patches or eyedrops that blur vision, gives the weak eye a competitive advantage and time to re-grow its afferent nerve connections. This regrowth potential decreases with age, and once a child reaches 7-10, very little can be done to improve the amblyopic eye.
How to Detect:
As you can imagine, you want to pick up amblyopia at an early age. Unfortunately, it is exactly these younger children who’s vision is most difficult to check. Pediatricians always check vision as part of a well-baby exam, and schools perform vision screenings – but vision assessment in children is tricky, even for trained ophthalmologists. We get many false-positive “poor vision” referrals from these sources, but that’s ok, because early detection is important!
 The word “lens” is named after the lentil plant (greek name Lens culinaris) whose 2 – 9 mm disk-shaped seeds bear a remarkable resemblance in size and shape to the human lens.
The word “lens” is named after the lentil plant (greek name Lens culinaris) whose 2 – 9 mm disk-shaped seeds bear a remarkable resemblance in size and shape to the human lens.
The lentil legume was one of the first agricultural crops and was grown over 8,000 years ago. Introduced in the U.S. during the early 1900’s, the “lentil bean” is grown in drier Washington, Idaho, and Western Canada and the seeds can be used in soups, stews, casseroles and salad dishes.
Strabismus:
Strabismus describes when the eyes are not aligned with each other, such as when an eye is turned in (cross-eyed or esotropic) or turned out (wall-eyed or exotropic). Here are some terms we use in ophthalmology to describe misalignments:
Esotropia (ET): The eyes are turned inwards (cross-eyed) all the time.
Exotropia (XT): The eyes are turned outwards (wall-eyed) all the time.
Eso/Exo-phoria: Phorias are eye deviations that are only present some of the time, usually under conditions of stress, illness, fatigue, or when binocular vision is interrupted.
Detecting Strabismus in babies
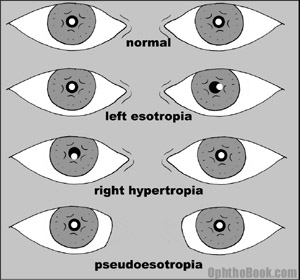 A quick way to check alignment inbabies is to shine a penlight into their eyes. You can determine alignment by looking at the corneal-pupil light reflex (the light reflection off the cornea) to make sure it is centered over the pupil of each eye. A large percentage of newborn infants will have some tropia at birth that goes away within a few months.
A quick way to check alignment inbabies is to shine a penlight into their eyes. You can determine alignment by looking at the corneal-pupil light reflex (the light reflection off the cornea) to make sure it is centered over the pupil of each eye. A large percentage of newborn infants will have some tropia at birth that goes away within a few months.
Don’t be fooled by pseudostrabismus – this is the illusion of crossed eyes caused by nasal epicanthal skin folds found in many Asian and young children. On casual inspection of these children, less white sclera is seen nasally and the child “looks cross-eyed.” However, closer inspection will reveal normal corneal light reflexes and no refixation on cover testing. Children outgrow these epicanthal folds as the bridge of the nose becomes more prominent.
With younger children who don’t track well, you can use the Hirschberg’s test – a quick method to estimate the amount of prism deviation in a misaligned eye. For every mm the corneal light reflex is off center, equals approximately 15 diopters of prism.
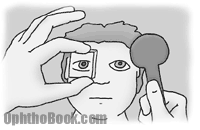 You can pick up phorias and tropias with the cross-cover test. Since the cross-cover test breaks binocular vision, the phoric eye will wander off axis when it has nothing to focus on. The amount of deviation can be quantified using prisms. This is a difficult technique to describe in words … basically you alternately cover the eyes with a paddle and hold up prisms until the deviation is neutralized. Detecting and measuring tropias and phorias is much more complicated then this, but I think this is enough for now!
You can pick up phorias and tropias with the cross-cover test. Since the cross-cover test breaks binocular vision, the phoric eye will wander off axis when it has nothing to focus on. The amount of deviation can be quantified using prisms. This is a difficult technique to describe in words … basically you alternately cover the eyes with a paddle and hold up prisms until the deviation is neutralized. Detecting and measuring tropias and phorias is much more complicated then this, but I think this is enough for now!
Strabismus as a major cause of amblyopia
If a child has misaligned eyes, they can unconsciously suppress one of their eyes to avoid seeing double. However, this suppression leads to amblyopia and permanent visual loss. Adults don’t have this ability to suppress vision and if they develop strabismus (such as from a nerve palsy or trauma) they will permanently see double.
Treatment of Strabismus:
Before taking anyone to surgery, correct all the non-surgical causes of strabismus: check for refractive error and treat any amblyopia – many cases of strabismus will improve or resolve by just doing these things. Eye surgery consists of shortening or relaxing the extraocular muscles that attach to the globe to straighten the eye.
Strabismus Surgery
To correct simple esotropias (cross-eyed) or exotropias (wall-eyed) we can weaken or strengthen the horizontal rectus muscles. A recession-procedure involves disinserting the rectus muscle and reattaching the muscle to the globe in a more posterior position. This effectively weakens the action of this muscle and turns the eye accordingly.
The picture below demonstrates the basic strabismus surgical technique – after exposing the rectus muscle from the overlying conjunctiva and Tenon’s fascia, you imbricate the muscle with double-armed vicryl suture, disinsert the muscle from the eye, then reattach the muscle to the globe via scleral passes at a measured distance from the original insertion. A resection procedure strengthens the muscle – you disinsert the muscle, cut off a section, and then reattach the muscle to the original insertion site.

The dangerous step with this surgery is reattaching the muscle – as you don’t want your scleral pass to run too deep and pierce the eye! Strabismus surgery isn’t technically difficult to perform, compared to cataract surgery, but it does take experience and good pre-op measurements to titrate the amount of recession/resection needed.
The goal of strabismus surgery is correct alignment so that the eyes are properly aligned when looking straight ahead and when reading. No surgery can “fix” the underlying muscle problems, such that the child may not have perfect alignment in all gaze directions.
Shaken Baby Syndrome:
This is a depressing topic (I won’t be adding any funny cartoons to this section). This terrible condition is important to recognize as it is preventable.
New babies cry a lot – on average three hours a day, and often for no apparent reason. Some babies cry significantly more than this! Frustrated caregivers may pick up the child and shake it if suitably irate. This shaking can become a reinforcing response as the infant becomes somnolent afterwards and stops crying, exactly the response the caregiver was hoping for. Infants are predisposed to physical damage from shaking as they have big heads and weak neck muscles. As the head whiplashes back and forth, the acceleration and deceleration forces traumatize the brain in a big way. Biological fathers and boyfriends are the most common perpetrators of this behavior, but anyone can be the attacker – this phenomenon spares no ethnicity, religion, culture, or social class.
These children are typically 5 to 10 months of age and present with somnolence, seizures or coma. The classic triad of exam findings include:
- Intracranial hemorrhage: usually a subdural hemorrhage secondary to tearing of the small bridging veins between the dura mater and arachnoid.
- Brain swelling: from shearing forces, diffuse axonal damage, secondary edema, and infarction.
- Retinal hemorrhages: specific findings (see below).
The child can also have other physical findings such as bruising of the body trunk (where the shaker grips the child) and fractures of the skull, long bones, or ribs. Remember: be suspicious for abuse when you see many bone fractures at different stages of healing.
Retinal Findings:
An ophthalmologist needs to be called in for any case of potential shaken baby to evaluate the retina. These kids have specific retinal hemorrhages that aren’t really seen in any other condition:
1. Large retinal hemorrhages located in all quadrants of the eye, located in all layers of the retina (subretinal, intraretinal, and preretinal).
2. Retinoschisis cavities. A schisis is a split between layers of the retina, and is very suspicious for abuse in this age group.
It’s imperative to write a descriptive note in the chart (have the attending write this note for litigation reasons) and document any bleeding with fundus photography. You want to take these photos soon, as hemorrhages can resolve in only a few days!
What about other causes of retinal bleeding?
Studies have found that household injuries, such as a fall from caregiver’s arms or furniture doesn’t usually cause significant retinal hemorrhage. Birth trauma can cause mild retinal bleeding but this is usually limited and resolves in the first few months. CPR with chest compressions rarely causes significant hemorrhaging. The hemorrhages in SBS are impressive and similar retinal bleeding isn’t seen except with big trauma such as a high-speed car wreck or a multi-story fall.
Be sure to look for any coagulopathy with basic lab testing, including CBC, coags, platelet count and bleeding time.
Prognosis:
While a third of these babies have no long term sequela, the long-term prognosis is generally bad. Twenty percent of these abused children die outright and the remaining kids end up with life-changing developmental problems, mental retardation, blindness, paralysis, and behavioral changes.
The Leukocoric pupil:
Every newborn receives a baseline exam by their pediatrician, and part of this exam involves checking for a good red-reflex off the retina. Leukocoria describes a white-colored pupil. This finding should concern you and requires an ophthalmology consult as the causes may be serious. Potential causes of leukocoria that you should look for include:
1. Congenital Cataract
2. Retinoblastoma
3. ROP (retinopathy of prematurity)
There are many other causes for a white pupil, such as persistent hyperplastic primary vitreous, but let’s focus on these three:
Congenital Cataract
A cataract in a newborn can occur by several mechanisms. They can be idiopathic, genetic, from metabolic disorders, child abuse trauma, or caused by one of the maternal TORCH infections during fetal development. Whatever the cause, it is important to remove these cataracts as soon as possible as they are amblyogenic and will lead to permanent vision loss from visual neglect. Replacing a lens is tricky, however, as babies are tiny, generate an impressive inflammatory response, and their “prescription” is still changing as the eye continues to grow. The cataract is removed as soon as possible, but often the lens implant can be placed at a later date – parents have to deal with aphakic contact lens or thick glasses in the meantime.
Retinoblastoma
Retinoblastoma is a tumor of the primitive retinal photoreceptors. The tumor grows on the retina and forms a white or cream-colored mass that can completely fill the eye, creating a white iris, and often a retinal detachment.
Retinoblastoma is the most common primary malignant ocular tumor in children. That being said, the cancer is still very rare, with only 250-500 new cases reported in the United States each year. You don’t want to miss this one, though, as failure to diagnose RB results in the death of a child.
These children are under 4 years of age, with the average age of diagnosis 18 months. There are different types of RB, and the tumor can arise from a random somatic mutation or develop along several germline inheritance patterns.
Treatment modalities are many, but decisive treatment often involves enucleation (removal) of the entire eye to avoid seeding tumor cells into the orbit. The tumor spreads by extension down the optic nerve toward the brain so it is important to get a good optic nerve section upon removal with careful microscopic evaluation for margin involvement. The overall survival rate in the US is very good, approaching 90%, but only if the tumor is recognized early.
Retinopathy of Prematurity
ROP is an important disease process that is commonly found in neonatal ICUs. Here’s how ROP works:
The retinal blood supply begins formation around week 16 of gestation, with retinal vessels springing forth from the optic disk and spreading outwards in an expanding fan toward the edges of the retina. By the 8th (36 weeks) month this vasculature has reached the nasal retinal-edge, and within a few more months the whole retinal blood supply has formed 360 degrees.
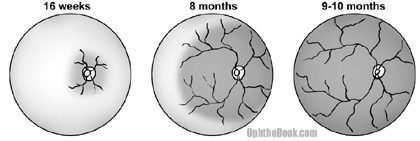
Everything sounds good, right? Well, problems can occur if a child is born premature. With premature eye metabolism, areas of peripheral retina that haven’t yet developed blood supply can become ischemic. Ischemic retina produces VEGF with resulting neovascularization. These neovascular vessels can bleed, create traction, and eventually retinal detachment. A leukocoric “white pupil” can result if the retinal detachment is big enough. The more premature a child is born, the more likely this unfortunate sequence of events is to occur. For this reason, children born under 32 weeks or less than 1,500 grams are screened to insure their retina is forming properly.
We treat these kids in a similar fashion as proliferative diabetic retinopathy in adults – PRP laser or cryotherapy is used to ablate the peripheral ischemic retina in an attempt to shut down excess VEGF production.
PIMP QUESTIONS
1. How is the Bruchner test performed? What will a near-sighted child look like with this exam?
The Bruchner test is a simple method to estimate the refractive error in a child. You look at a child through your direct ophthalmoscope from a distance. Light up the face such that both pupils are lit. Hyperopic children will have superior crescents in their red-reflex, while myopic (near-sighted) children will have inferior crescents.
2. How do you determine the refractive error (glasses prescription) in a pre-verbal child?
By streak-retinoscopy. This is where you flash a light beam across the retina and hold up different lenses in front of the eye until the red-reflex movement is neutralized. Correct for your working distance and you have your prescription.
3. What is amblyopia? What causes it?
Amblyopia is poor vision in an eye from disuse at an early age, usually secondary to strabismus or an unrecognized refractive error.
4. How do you treat amblyopia?
You treat by “penalizing” the good eye. Using a patch over the good eye forces the amblyopic eye to work. Also, you need to treat any underlying cause of the amblyopia such as anisometropia.
5. You suspect a baby of having strabismus, but because of the baby’s age you aren’t able to measure eye deviation with your prism set. How can you estimate the amount of eye deviation?
You can do this by measuring the corneal light reflex in relation to the underlying pupil (Hirschburg test). For every millimeter of light deviation, you have approximately 14 diopters of strabismic deviation.
6. What’s the difference between a tropia and a phoria? How can you differentiate this on exam?
This is exactly the kind of question you’ll get asked during a pediatric or neuro clinic. A tropia is a deviation that is there ALL the time. A phoria is intermittent, and tends to occur more with fatigue or when one eye is covered.
As for how to pick these up: it’s hard to describe, so you should have one of the residents demonstrate how these are done:
Tropias: cover-uncover test
Phorias: cross-cover test
7. The actress Lucy Liu (from Charlie’s Angels) brings in her new baby. The Asian American actress is concerned because Drew Barrymore said her baby’s eyes look “crooked.” Casual inspection shows a healthy 12-month old baby who appears mildly esotrophic (cross-eyed). How would you measure ocular alignment in this child.
You can check the corneal light reflex with a penlight.
8. The corneal light reflex appears to be correctly centered (normal Hirschburg), yet the child still looks esotrophic. In fact, the child looks a lot like her attractive Asian mother. What’s going on?
This sounds like pseudostrabismus from epicanthal folds. The nasal skin creates the illusion of crossed-eyes as less white sclera can be seen nasally. As babies get older, the nasal bridge becomes prominent and this appearance usually goes away.
9. What systemic and eye findings will you see with shaken baby syndrome?
In the eye, you will see retinal hemorrhages at “all levels of the retinal in all four quadrants of the eye.” Schisis cavities (large splits within retina layers) are relatively specific. Other system findings include intracranial hemorrhage, brain edema, and skull-rib-long bone fractures. On exam you might also find bruising on the body trunk and under the armpits. Supposedly, these kids can have a torn frenulum (the piece of tissue under the upper lip that connects the lip to the gumline), but I’ve never seen this myself.
10. Parents say that a child fell from her crib and hit the floor. Do you think this would cause a fracture and the retinal findings of shaken baby?
Kids are relatively bouncy, but this story COULD account for the skull fracture. However, it takes a LOT of traumatic force to create large retinal hemorrhages — this story sounds a little fishy. An experienced pediatrician and ophthalmologists needs to examine this child.
11. Name three causes for a leukocoric pupil.
Cataract, retinoblastoma, and retinopathy of prematurity.
12. List risk factors for developing retinopathy or prematurity.
Gestational age less than 32weeks, birth weight under 1,500 grams, and systemic hypoxia.
13. How soon should a congenital (found at birth) cataract be removed?
Soon, in order to avoid amblyopia. Some recommend removing these early cataracts in the first two months.
My Neices baby at 2 months of age has been diagnosed with opthalmic folds. The babies eyes both constantly twitch or move from side to side.
He does have sight but can you please eplain to me. He has been referred to a laser specialist in Sydney, Australia.
Editors Notes: Hard to say, as I’ve never heard the term “ophthalmic folds” … a couple of possibilities. One is that he has retinal folds, possibly from retinopathy of prematurity, thus prompting the referral to a laser (retina) specialist. The roving eye movements sound like either a congenital or sensory nystagmus. Be sure to followup with the doctor in a timely manor and make sure they explain to you exactly what’s going on. Sometimes it helps to have your doctor write the diagnosis down on a piece of paper so you can research it.
Hola soy de Ecuador, estudio Optometria, quisiera que me ayuden con un video de Estudio de las Condiciones motoras (Test subjetivos: Diploplias de Willians, Pantalla de Lancaster- Metodos mixtos)
Si tienen este video envienlo a mi mail para exponerlo en clase gracias…
you are a very talented ophthalmologist
My Daughter is 9 years old and her eyes deviate equally to the sides gradually and stay deviated when she is watching the television. Her vision is otherwise good and no deviation of the eyes and neck when in the class room or when doing other activities. Upon questioning she says that she cannot see properly the image on the television when she looks straight and she has to deviate her eyes and eventually the neck. We have seen a pediatric ophthalmologist regarding this at the age of 9 years and upon his exam he says that it is torticollis.
He wants to do another exam after the dilatation in 6 months.
Do we call this esophoria or is there another term for this.My concern is that is it going to cause amblyopia/ vision problems in the future.
Thanks,
Chandra
hello, my daughter who just turned 4 has a hemorage in the right eye that rebleed yesterday as of right now shes on 3 different drops is there anything else i can do. and is treatment differ from a child to an adult. thanks very concered tammy
My four year old child turns her head to the left and looks from the exteme corner of her her eyes when looking at distance especially when watching television. One doc said it was fourth nerve palsy but three others disagree. She sometimes complains of a black spot in the middle of the television that goes away when she turns her head. If it’s not fourth nerve palsy, what could be the problem?
Hi,
Correct spelling is Bruckner reflex. Great site. Can i recommned it to my med students?
hi, my baby just turned 6 months..
and i don’t know if her eyes are crossed or it’s just because she’s still a baby… she is half western half asian baby.. could it be because her eyes looks like asian? i hope to hear some answers… thanks.
Hi, correct spelling in pimp questions 5 and 8 is “Hirschberg test”.
Thanks
I live on prince Edward Island canada where can we find a
Pediatric Ophthalmology in the general area like Nova Scotia or New brunswick
thanks for you time
my son was born at 24 weeks gestation. because of his prematurity his lungs were very underveloped and required him to be on high levels of oxygen which caused his retinopathy. he wears very thick lensed and I would like to know if it is possible for him to have surgery when he is older to restore some of his vision?
Hi, My son who is now 5 was born at 23 weeks gestation. He developed ROP, had the corrective laser eye surgery and has been seeing an opthamologist ever since. He is very short sighted in his right eye which is also “lazy” or turning in. As such we are having to put dilating eyedrops in his left eye to encourage him to use his right eye. Anyhow I took a photo of him today and noticed that in the photo his dilated pupil had a yellowy-red crescent shape in the photo. I have heard and read about people detecting eye cancers in kids eyes after using flash photography and am now worried that that may be what I am seeing in this photo. Please contact me with your opinion on this as we don’t have another eye appointment for three months and I know a quick diagnoses can be important if it is cancer. I can send you the photo to look at. Thanks you.
thanks sir, ur lectures and videos was so great,easily presented,
in video of this chapter, u wrote abt risk factor for ROP > babies less than 1500 kilograms(kg).
but ur pdf text if correct
thanks 🙂
my 2 years10 months daughter is suffering from mild squint. our docter suggest us a spects and said that her both eye sight no is spherical +1.75 and told us that every child have low eye sight. Is every child have low eyesight and mild squint will be recover by own or when child become older then the quint recovered by own. please tell me the treatment. and why squint happend to our child
my son aged 4has started to twitch( raise forehead and eyebrows) when watching tv and when i’m reading stories to him, any ideas what this might be?
my son aged 4 has started to twitch repeatedly when watching tv and when i read to him, any idea what this might be?thanks
My 18 month old son started about a month ago when he is playing will stop what he is doing and his eye will go up and to the left and he will blink a lot, when he stops blinking his eyes will stay there for a little bit, then he will stop and go back to playing, any idea what this is? He don’t do it everyday, and when he does it he acts like he didn’t even do anything. Thanks.
Hi, My 3 month old seems fine but when i cover her right eye she freaks out but is okay when i couver her left eye. she follers things like my finger on ther right side but does not do the same with her left eye. she doesnt evemn turn her head when we talk to her from the left side. Her left eye may also look a tad smaller and when she was about a month old she had a blocked tear duct. What could be wrong o is something wrong please help
My son aged 4years have diagonosed for patch one eye.And +5D spy. Glass to wear what is the cause of poor vision and is there any chance to improve vision.
HOLA MI HIJA TIENE UN MES DE VIDA Y TIENE UNA DESVIACION DEL OJO IZQUIERDO. ES PERMANENTE SU DESVIO. ME GUSTARIA SABER QUE TRATAMIENTO TENGO QUE REALIZARLE, Y PORQUE ES SU DESVIO MUCHAS GRACIAS ESPERO UNA RESPUESTA. YA QUE ES MUY IMPORTANTE LA VISTA DE MI HIJA.
MY SON AGE 5 MONTH HE FALLINGS TEAR EVERY TIME ON RIGHT SIDE EYE PLS. WHT I DO
Dear Dr Root,
Just found your videos online. Wonderful
I need your help to design a brochure and video for working with kids with autism. I am an ophthalmologist, do alot of international work and local in Kansas with this population. If you could send me your email so we can correspond. I could not find on your website.
I am AAO member and AAPOS member you can check me out….
Linda Lawrence MD
Salina, Kansas
very good . thanks
dear diana
check with your pediatrician. your child may be having absence seizures.
Arlene, Rn
CT.
Thanks a bunch for sharing this with all people you actually understand what you are speaking about! Bookmarked. Kindly additionally discuss with my web site =). We will have a link trade arrangement between us
Hi. My dd is now 2 and was a 28 weeker. She has a weak eye which is not responding to patching. She manages well with patch on, but in the dark with patch, struggles. At recent review retinal folds or crease was mentioned and further investigation under sedation is requested. If it is a fold or crease, can her vision in this eye be improved? She has a small white patch in her pupil of her weak eye. To make matters worse, she also was born with congenital toxoplasmosis and has chlororetinal scars, but not in her field of vision. These exist in both eyes. She has no developmental delay and does not appear to be limited by vision problems, but accept she is not at reading age as yet etc. any advice please? Thanks
Aly,
Your questions are pretty specific and need to be answered by a pediatric or retina ophthalmologist. At the very least, it sounds like an exam under anesthesia is required. As far as prognosis … I have no idea.
my friend is belong to an indian and she is settled in UK her baby was born with lack of eye reflex.Is it normal for asian babies?……
My daughter is 7.5 weeks old. I had noticed a slight drift in her eyes a couple weeks ago, then during early morning feedings I saw one eye or the other drift quite a bit outward. Now that she has become more visually aware, I have noticed over this weekend that this is happening more frequently, for longer duration. There are times when she will seem to focus just fine, and she also follows with her eyes, objects and faces (parents and siblings!) The outward drift is intermittent. So far. I will take her to her doctor tomorrow, but I wonder if he will see what we see. Is it TOO early to detect a problem? Is it too early to treat? How can I make sure she gets treatment if it is needed?
Hi, my 11 year old boy is developing something like a fold/pimple in his eye..just between the iris and the sclera.For a day i saw a fold now its starting to be red. He doesn’t show any signs of itching and doesn’t cry too.What do you think it is? please help.
Hi, my 11 month boy is developing something like a fold/pimple in his eye..just between the iris and the sclera.For a day i saw a fold now its starting to be red. He doesn’t show any signs of itching and doesn’t cry too.What do you think it is? please help.
My grandsons eyes are constantly moving in quick jerky back and forthmovements. They are telling us to wait till feb apt. There is no way he can possiblyfocus like this. They say his optic nerve is weak.what does this mean? And will he be able to see?
Thanks for some needed answers
vickie
Vickie:
1. Make sure your grandson sees a “pediatric ophthalmologist”
2. Ask the pediatric ophthalmologist if the child needs an MRI to rule out optic nerve tumor
Beyond this, I don’t have any answers for you. Pediatric nystagmus management is out of my practice area.
When my baby turned 6 mo her pediatrician asked me if i took pics of her with flas on because when she examin her noticed some ‘condition’ on her right eye, i told her i dont use flash on her and asked if she was ok, she said it was a ‘rare’ condition but should be fine. My baby is one yrl old now and i notice she shows white pupil and not red on a fee pics i have used flash. Im not sure if its the angle or if i should take care for a checkup i Dont have a su gle photo with red eyes.
Diana, you need to take your child to an actual eye doctor for a dilated eye exam. There is no way to diagnose this problem online.
I’m 29, and I was born with a congenital cataract to my right eye. I had a keratophakia when I was about 1 year old. During my early childhood my mom would attempt to do the patch as was ordered by the doctor. Unfortunately I now have very very poor vision with amblyopia mostly with far sight, and cross eye at very near sight. My right eye provided me with great peripheral view at least. Since the age of 10, my ophthalmologist has diagnosed glaucoma, or not sure if the corneal transplant is having an effect on the pressure reading. Just yesterday my pressure was 32, that’s without me taking my eye drops for quite some time. Just wondering what your thoughts/insights may be on the pressure reading validity post a keratophakia at the age of 1. My opthamologist isn’t sure. This has been a life long challenge, that I continue to struggle with. Thanks in advance for your time.
Very Nice URL to understand thing. I am Parents of child – myophic… really nice information